Pain is subjective. No one but you knows how you really feel. When you have RSD, pain is at the core of your treatment and medications. Nurses and doctors constantly ask you to measure your pain on a scale of 1 to 10, or by pointing to a series of faces.
What do you do when your pain doesn’t fit on a scale?
Daily I find myself trying to assess my pain and put it into the box that has been identified by the medical community as the pain scale.
But my pain is so far beyond a 1 through 10 or a face that it has a painter expression. So I start assessing whether I can get out of bed that day. Or if my Orthostatic Hypotension will cause me to become more unbalanced then I already am. I try to put that internal pain assessment into the numbered scale I’m given.
But really, here’s everyone else’s pain scale:
Numerical rating: Usually based on a scale from 0 to 10, this scale assigns a measurable number to your pain level. 0 represents no pain at all while 10 represents the worst imaginable pain. Wong-Baker: Represented by faces with expressions, this scale follows the same guideline as the numerical scale. 0 is represented by a smiley face, while 10 is represented as a distraught, crying face. This scale is useful when rating pain in children, or for adults with mild cognitive impairments.
Wong-Baker: Represented by faces with expressions, this scale follows the same guideline as the numerical scale. 0 is represented by a smiley face, while 10 is represented as a distraught, crying face. This scale is useful when rating pain in children, or for adults with mild cognitive impairments.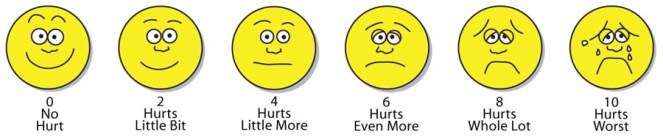 And here’s mine:
And here’s mine:
The McGill Pain Questionnaire consists of groupings of words that describe pain. The person rating their pain ranks the words in each grouping. Some examples of the words used are tugging, sharp and wretched.
Once the person has rated their pain words, the administrator assigns a numerical score, called the Pain Rating Index. How do you even begin to try to put the two together?
How do you even begin to try to put the two together?

